
Study: Cannabinoid Use in the Treatment of Osteoarthritis Pain
What is Osteoarthritis?
Arthritis is the inflammation and swelling of joints, the area where bones connect, which provide support to the body and assist in maintaining mobility. Osteoarthritis is the most common type of arthritis and is caused by “wear and tear,” or long-term use (the other type of arthritis, rheumatoid arthritis, is caused by an overactive immune response in the body). In some cases, it may have a genetic basis.
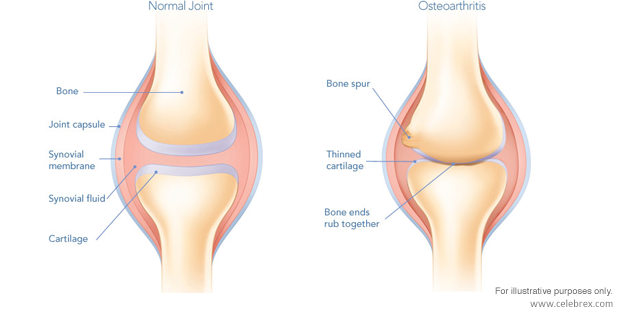
This long-term use results in destruction of hyaline cartilage, a firm connective tissue found in joints that prevents bones from rubbing against each other and getting damaged. Joints of the body most commonly affected by osteoarthritis are the hands, knees, hips and spine, and symptoms include pain, swelling, and stiffness. Osteoarthritis is the cause of approximately 69.9% of hospitalizations (approximately 814,900 in the United States in 2006) that result from arthritis complications.
As a result of the large range of activities people perform on an everyday basis using their joints (e.g. holding a cup, writing, typing, turning on a faucet, tying shoelaces, eating, walking, kneeling, squatting, bending, etc.), symptoms can be severely debilitating, significantly interfering in the lives of patients who suffer from it. According to the CDC’s osteoarthritis website:
- [Osteoarthritis] of the knee is 1 of 5 leading causes of disability among non-institutionalized adults.
- About 80% of patients with [osteoarthritis] have some degree of movement limitation.
- About 40% of adults with knee [osteoarthritis] reported their health “poor” or “fair.”
Osteoarthritis can also lead to shortened survival, both directly and as a result of treatments required for management (e.g. bleeding of the stomach caused by NSAIDS, a type of over-the-counter anti-inflammatory medication). The economic burden of osteoarthritis, including costs associated with knee and hip replacements and efficiency loss in the workplace, is over $50 billion.
Exercising regularly and maintaining a health weight can help prevent osteoarthritis from worsening, and may reduce symptoms of osteoarthritis, such as pain and joint dysfunction.
Study Results
An animal study published in PloS ONE found that cannabinoid (CB2) receptor stimulation in the spinal cords of rats acting as models for osteoarthritis pain in humans (treated with monosodium acetate to induce osteoarthritis-type pain and joint issues) led to decrease in pain response and inflammatory markers.
In the rat model for osteoarthritis pain, researchers found:
- an increase in CB2 receptors in neurons and microglia (essential supportive cells for neurons)
- markers of central sensitization (i.e. a heightened response to pain as a result of pain neuron “irritation”/activation by surrounding tissue damage or swelling) including spinal astrogliosis (an increase in overactive astrocytes [supportive cells of the nervous system]) and increased activity of metalloproteases (connective tissue degrading enzymes) in the spinal cord
- the presence of more severe knee cartilage disease was associated with a decreased amount of CB2 mRNA (a receptor-making template)
Resultsof cannabinoid stimulation included the following:
- JWH133, a compound that stimulates CB2 receptors (i.e. a CB2 agonist) helped to reduce behavior associated with pain and spinal neuron response to pain stimuli, and prevented increases in IL-1β and TNFα (inflammation markers).
- Administration of the CB2 agonist directly to the spine helped to prevent osteoarthritis-type pain responses.
- Administration of the CB2 agonist reduced central sensitization.
Conclusion
According to the researchers, “Targeting CB2 receptors may have therapeutic potential for treating [osteoarthritis] pain.” Therapies that stimulate CB2 receptors, including endocannabinoids, phytocannabinoids, or synthetic cannabinoids, may prove useful to this end.
Not only do these results add to previous evidence suggesting that cannabinoid therapies may be useful in the treatment of pain (e.g chronic and neuropathic pain, as well as pain resulting specifically from osteoarthritis and rheumatoid arthritis) and inflammation, but according to the researchers, they also “provid[e] a neurobiological basis for analgesic effects of the CB2 receptor” (i.e. the effect of cannabinoid therapies on pain are unlikely to merely be a result of emotion regulation).
“Targeting CB2 receptors may have therapeutic potential for treating [osteoarthritis] pain.”
Given that (1) opioid prescription is a pain management option for patients with osteoarthritis for whom standard therapies are not optimally effective or are contraindicated (i.e. they must be avoided), (3) use of opioids can lead to severe negative side effects, abuse, dependence, and death, and (3) cannabis use may be able to partially (as an add-on therapy) or fully replace opioid use in some instances, patients may benefit from access to alternative, safe pain management options like cannabinoid therapies.
Cannabinoid therapies have a favorable safety profile, patients with osteoarthritis have a significantly decreased quality of life as a result of their symptoms, and the burden for patients translates into large financial losses. Therefore, finding safe alternative ways to manage the symptoms of osteoarthritis for patients who are not experiencing optimal relief from standard therapies, or who are experiencing significant negative side effects from standard therapies that could be partially replaced by cannabis use, is essential.
For information on reasonable expectations and safety in considering whole-plant medical cannabis use, as well as how you can advocate to move cannabis out of the Schedule I controlled substance classification in order to increase research on phytocannabinoids in the United States, click here.